Of all the interventions that anti-aging medicine has brought to patients who wish to slow the aging process, human growth hormone (HGH) is arguably the most profound and the most controversial.
HUMAN GROWTH HORMONE Therapy (HGH)
Hormone Therapy Right For?
For all information on hormone therapies please email Dr. Steve Zakany at [email protected]

What is Human Growth Hormone?
Human growth hormone, also known as somatotropin, is the most abundant hormone made by the pituitary gland in the brain. Cells in the pituitary, known as somatotropes, produce HGH and release it into the bloodstream, where it can have a direct effect by itself on tissues and organs, or it can be absorbed by the liver and converted into various other growth factors. HGH is released in pulses throughout the day, determined in large part by “circadian rhythms.” Most HGH release occurs during stages III and IV deep sleep.
Two hormones, GHRH and somatostatin, produced in the hypothalamus regulate HGH production through a feedback loop. Growth hormone-releasing hormone (GHRH) stimulates HGH production and somatostatin inhibits HGH production. Specific gastrointestinal cells produce third regulating hormone, Ghrelin, which works in synergy with GHRH to stimulate HGH production.
More Information
Human Growth Hormone obtained its name from the fact that HGH is necessary to make children grow in stature. At one time, this was believed to be essentially the only role played by HGH. We now know differently. It appears that nearly every organ in the body depends on Human Growth Hormone for proper growth and development as it increases anabolic activity and lean body mass. It regulates the body’s metabolism of proteins, electrolytes, carbohydrates, and controls how the body uses fat.
The muscle building actions of growth hormone don’t come from growth hormone directly but are mediated by conversion and release from the liver of a more potent and active form, called insulin-like growth factor 1 (IGF-1). HGH also causes the body to produce binding proteins that carry IGF-1 and act as hormones in their own right. The pituitary gland secretes growth hormone in brief spurts, and disappears from the blood very rapidly, making direct measurement next to impossible. Instead, IGF-1 levels do not fluctuate as rapidly, making it a surrogate marker of HGH levels.
Human Growth Hormone Benefits
Benefits
HGH has also been shown to:
-
Help lower blood pressure
-
Help lower cholesterol
-
Decrease insulin resistance
-
Improve bone density
-
Increase lean muscle mass
-
Increase skin health
-
Slow hair loss
Side Effects of HGH?
There have been no reported significant effects on the hormones that are derived from pregnenolone, even in high doses. Nevertheless, conversion to DHEA could theoretically cause acne and hair loss, especially in women.
If any of these symptoms occur, discontinue the pregnenolone for one week or until symptoms resolve and notify your physician, then resume at one-half the previous dose.
(©Gregory W. Petersburg, D.O. All rights reserved. Living Younger, pp. 145-146.)
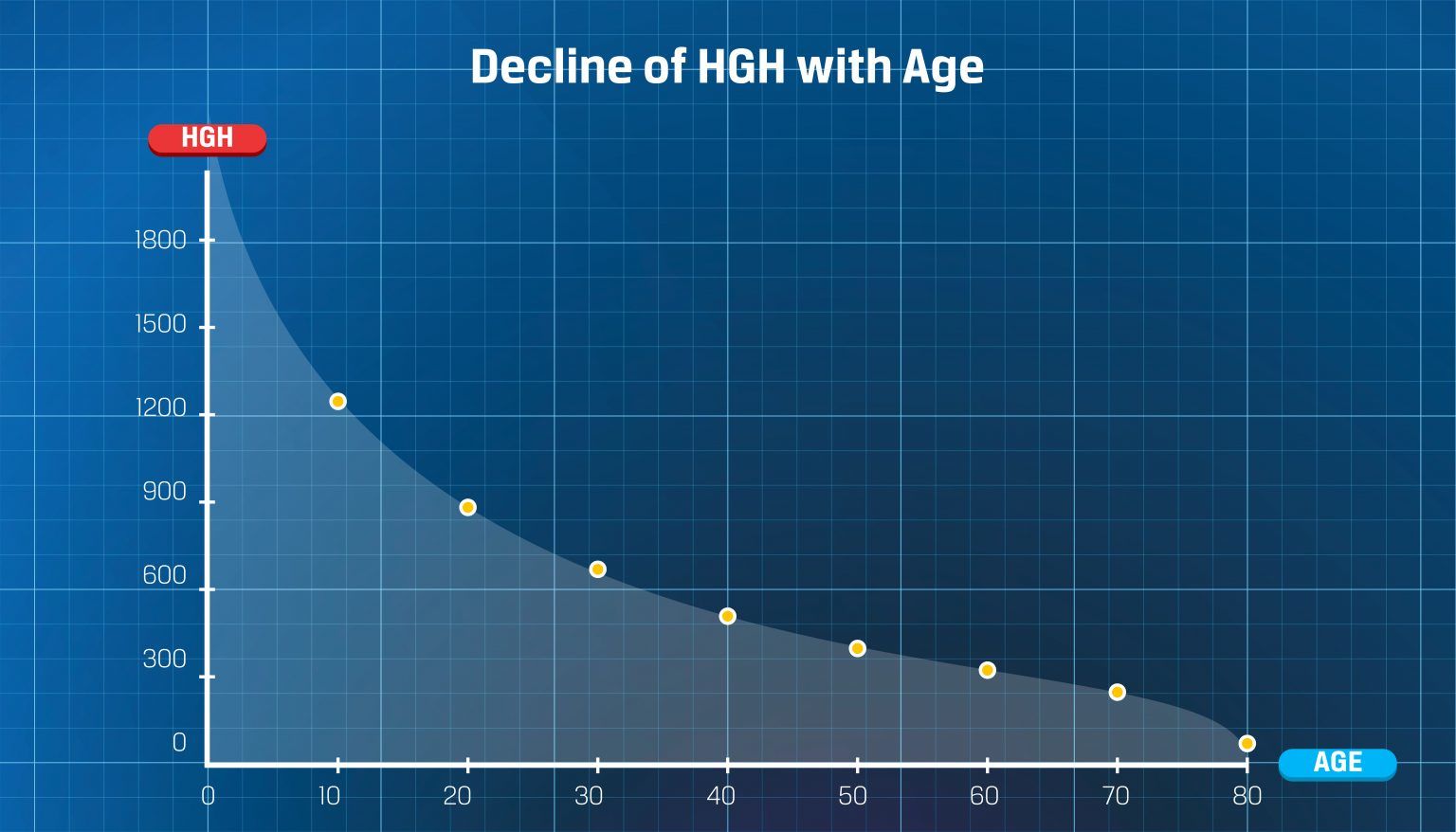
HGH Decline with Age
Human Growth Hormone of HGH is a very important hormone in the body. Doctors believed for years that HGH decline with age was a natural part of aging. However, processed food, weight gain and stresses of the 21st century have caused doctors to see a deeper, sharp decline of Human Growth Hormone levels at younger ages.
Hormone Therapy Costs
Comprehensive Blood Panel
$ 250
One TimeBio-hormone Appointment & Care Plan
$ 500
(includes the first 6 months of follow-up)Hormone Management
$ 750
Annually (Labs and hormone cost not included)Hormone Therapy Details
The Master Hormone HGH
HGH has repairing and restorative abilities which can reverse the damage and facilitate re-growth of failing organs. It is unclear, however, whether maintaining physiologic levels of HGH or IGF-1 equivalent to those of a 25- to a 35-year-old person will extend the length of human life. But it is worth noting that the Journal of Clinical Endocrinology and Metabolism reported in 1997 that healthy centenarians have high serum IGF-1 concentrations.
Human Growth Hormone levels decline with age. After the age of 25, levels begin to decline at a rate of 10 – 15% per decade. As the levels of growth hormone decrease with age, so do the levels of IGF-1, falling by nearly 50% after the age of 40. The decline in HGH is known as somatopause.
Every hormone has a ‘pause’ and human growth hormone is no different.
(©Gregory W. Petersburg, D.O. All rights reserved. Living Younger, pp. 183-184.)
DHEA
DHEA levels decrease progressively from a peak at age 25 to less than 20% of that peak before the age of 70. Many people over the age of 40 produce inadequate levels of DHEA. Levels are typically low in those with chronic diseases such as obesity, diabetes, deficiencies, cancer, high blood pressure, heart disease and AIDS. Elevated insulin levels decrease DHEA levels; one reason why hyperinsulinemia increases vascular disease.
(©Gregory W. Petersburg, D.O. All rights reserved. Living Younger, pg. 139.)
Melatonin
Melatonin is produced naturally in the body, by the pineal gland in the brain. It is a fundamental regulator of the body’s inner clock, or circadian rhythm, which determines the 24-hour sleep/wake cycle. Levels are higher at night, are suppressed by bright light, and decline as we age. The length and height of the melatonin peak at nighttime determines the circadian phase of the biological clock and governs vital body parameters such as the variation of hormone levels, body temperature and sleep-wake cycles. Hormones such as estrogens, testosterone, DHEA, growth hormone, and cortisol are subject to circadian fluctuations. Over 100 body functions fluctuate over a 24-hour period and are dependent on sunlight and darkness as cues.
Melatonin derives from the essential amino acid L-tryptophan. Tryptophan, consumed in foods we eat (especially turkey and milk), is converted into the neurotransmitter serotonin, and is then further metabolized into melatonin at night. Melatonin levels are higher at night because bright light suppresses melatonin production.
The pineal gland is important, for not only producing melatonin but it also helps in restoring the thymus gland. The thymus gland, located in the upper chest, is a player in immune function by producing T-cells and natural killer cells. Unfortunately, the thymus begins to shrink drastically after about the age of 12. Because of the pineal gland’s direct effect on the thymus gland, replenishing adequate melatonin levels may improve immunity.
As we age, melatonin levels decrease. That is one reason why older people sleep less, even though they need the same amount of sleep as they did when they were younger adults. By about the age of 45 the pineal gland runs down. While melatonin secretion slowly declines over many years, in middle age the hormone level plummets.
(©Gregory W. Petersburg, D.O. All rights reserved. Living Younger, pg. 141.)
Pregnenolone
Pregnenolone is a hormone produced in the mitochondria in the brain, gonads and the adrenal glands. It is derived from cholesterol, and is a precursor for the biosynthesis of steroid hormones.
Pregnenolone and Sex
Pregnenolone has been called the mother of hormones because it is the precursor hormone to cortisol, progesterone and to DHEA, which is a precursor to the sex hormones testosterone and estrogen. Pregnenolone can be found in greater concentrations in the brain than in any other organ in the body and serves to enhance all our mental functions. As we age pregnenolone levels decline in the body as much as 60% by the time we are 75 years old.
On its own, pregnenolone is essential to keeping brain function at its peak capacity. However, male and female bodies use pregnenolone differently. In women, more of the pregnenolone becomes estrogen while in men more is used to make testosterone. For this reason, men with prostate conditions should use pregnenolone with caution. Pregnenolone replacement can raise progesterone levels in women as well.
Memory enhancement has been observed in humans and animals when given pregnenolone. Pregnenolone reinforces neurotransmitter systems that decline with age. It stimulates release of acetylcholine in the hippocampus of the brain, facilitating memory processes. It may also be an important component in repairing the fatty layer that protects nerves, known as the myelin sheath. Pregnenolone may also have a protective action against the unwanted effects of elevated levels of cortisol, our stress hormone. There as yet unsubstantiated claims that pregnenolone is useful in some forms of cancer and arthritis, in degenerative diseases associated with aging in general and in obesity. Current research is being done to test pregnenolone’s ability to help those suffering from Alzheimer’s disease, multiple sclerosis, cardiovascular problems and for boosting the immune system.
Cautions with Pregnenolone
Because pregnenolone is a precursor hormone to estrogen and testosterone, those with prostate, breast and uterine cancer should avoid pregnenolone replacement.
Thyroid
The thyroid gland is located in the neck, below the larynx, known as the voice box. The thyroid gland affects every function in the body because it controls metabolism.
What does the Thyroid do?
Thyroid hormones regulate the entry of oxygen into the cells, thus controlling metabolic rate, body temperature, brain maturation in neonates, heart rate, hair growth, ovulation, skin turnover, growth and development. Additionally, thyroid increases protein synthesis.
stimulating hormone (TSH) is produced by the pituitary gland in the brain and stimulates the thyroid gland to produce T4 (thyroxine). T4 is the primary hormone secreted from the thyroid gland. The liver and other tissues convert most of it to T3 (triiodothyronine), the more active form. T4 crosses the blood-brain barrier, but T3 does not. Some T4 also converts to metabolically inactive Reverse T3, more so with age.
- CRP, a marker for inflammation, increases with low thyroid function
- Thyroid hormones play a crucial role in normal cardiovascular function
- Smoking, a toxic environment, stress, chronic antibiotic therapy, congenital defects, genetic disorders, infection, nutritional disorders, radiation, hormonal imbalances (e.g., HGH) and tumors can all affect thyroid function
(©Gregory W. Petersburg, D.O. All rights reserved. Living Younger, pg. 147.)
Peptide Therapy
Due to the high cost of HGH, sometimes over $400 monthly, we generally recommend Peptide Therapy as another alternative.
Contact US
2299 Pearl Street, Suite 204 Boulder CO 80302
Monday – Sunday: 9:00 am – 6:00 pm
Please call for an appointment or consult


